by Linda L. Esterson, photography by Sarah Wockenfuss
It gets to a certain point and Sheryl Hockstra raises the white flag.
It feels like there’s a sword piercing through her eyeball to the back of her head. She stops what she’s doing, sits on the sofa and leans on a propped pillow. Sheryl stays in this position for at least two hours, allowing her migraine prescription to start working.
According to the American Migraine Foundation, one in four U.S. households includes someone who suffers from migraine, and a total of 1 billion people worldwide. This includes one in five women, one in 16 men and one in 11 children.
Amanda Harbert, a certified nurse practitioner with Carroll Health Group Neurology, says a migraine is a bad headache intensified by other symptoms like nausea, vomiting, light and sound sensitivity, dizziness and feeling ill. And the head pain is severe. Harbert calls the phenomenon migraine syndrome.
“I see people in all walks of life with headaches based on the hours they keep, their family life and what they take in for food and drink,” she says.
Cari Pierce holds certifications in several areas, including as a holistic health coach and personal trainer. She is the owner of Flip Yours Fitness and Wellness in Westminster. Pierce attributes migraines to inflammation and a heightened level of excitability of the neurons in the brain, which transmit information to other nerve cells, muscles and glands.

Migraine “is so widespread because we are super stressed-out people,” she says. “We try to do so much for so many, all day long, day after day. We’re a go-go-go society.”
The central nervous system can only handle so much, and when it’s overloaded it reacts, often as a migraine, Pierce explains. “Stressing the central nervous system puts the body on high alert. It’s our fight-or-flight response.”
Migraines also tend to run in families, and the Hockstra family is no exception. Sheryl Hockstra’s husband, Gerrit, suffers from severe headaches that come on as a result of weather and are handled with a medication that is effective in 15-20 minutes. Sheryl finds hormonal shifts related to her menstrual cycle can trigger migraines. Their daughter Leah, 17, deals with her migraines from both cycle and bariatric pressure shifts. Add the worry about schoolwork and her upcoming departure for Arizona State University, and she’s dealing with the pain often.
Leah recalls her first severe migraine at about 8 years old, during a trip to the movie theater. She returned home to cover her entire body with a blanket to shield herself from light. Today, she experiences symptoms a few times a week. Her medication, too, takes about two hours to take effect. She will shut herself off, cover her eyes and wait.
“I get a lot of pressure on the bridge of my nose between my eyes,” she says. “My eyes strain a lot. It hurts behind my eyes. The feeling of pressure in my head is sharp.”
In addition to stress and the hormonal and weather changes the Hockstras face, other factors can contribute to migraine level headaches, according to Harbert. These include a low quality or quantity of sleep, alcohol, dehydration, skipping meals and allergies, as well as trauma and tumors.
Many individuals can work through mild symptoms for a few hours, but if they are severe, sufferers may be forced into a dark room where they can do nothing but rest or sleep for up to a few days.
Harbert listed three levels of treatment for migraine. First is a lifestyle evaluation of sleep, diet, hydration and exercise (see sidebar), aimed at reducing the severity and frequency of headaches.
“Our job as animals in our environment is to recognize threats and survive them,” Pierce adds, noting unhealthy foods, bad choices and “the whole rat race” as contributors. “We’re a pretty stressed-out species. We wear stress like a badge of honor. We talk about being busy and better than [others].”
Pierce recommends a holistic approach, which incorporates many of the same lifestyle evaluations to take responsibility for the body.
“We have to be buffered with down time,” she says. “The nervous system is not meant to be on all the time.” Providing periods of relaxation, sleep, happiness and calm can help reset the brain and allow the nervous system to wind down. She also suggests paying close attention to nutrition and food sensitivities, which may also contribute to migraines.
When headaches are migraine-level, Harbert suggests what she calls “rescue therapy.” This consists of over-the-counter medications such as ibuprofen or acetaminophen or Triptan medications such as Sumatriptan and Eletriptan. These reduce inflammation to blood vessels and the trigeminal nerve, which wraps around the head. If headaches are frequent or severe, Harbert opts for prophylactic options, aiming to prevent the headaches. Clinicians are also turning to new therapeutic injections like Botox to block pain fibers from activating pain networks in the brain, and Aimovig, which blocks the calcitonin gene-related peptide (CGRP) receptor to prevent migraines. Also, preventative medications like Topiramate, Propranolol, and Trazodone are utilized.
Herbal supplements, including riboflavin and magnesium, can also help. According to Pierce, 75 percent of the population is deficient in magnesium, which has been proven to prevent migraines. She also suggests vitamin B, notably B6, which develops in the creation of neurotransmitters, and other supplements like 5-Htp, an amino acid that helps produce serotonin, a contributor to well-being and happiness.
“It’s about nourishing the body and giving it what it needs to function,” she says.
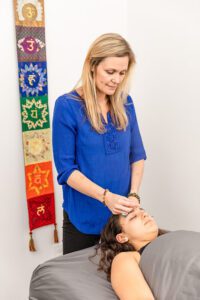
Another holistic approach is acupuncture, one of the oldest forms of medicine, says Jamie Schmidt, L.Ac., M.Ac., owner of Let It Be Acupuncture and Wellness in Westminster.
“Acupuncture is used to rectify imbalances of the energy life force known as qi,” she says. The treatment utilizes tiny needles to bring energy flow to the “proper” balance to allow the body to heal from disease.
Acupuncture can help in both the prevention and treatment of migraines. Many insurance companies now are covering acupuncture treatments for migraine sufferers.
Migraine Prevention and Treatments
- Pain medications – over-the-counter or prescription-strength
- Preventive medications
- Vitamin and herbal supplements
- Injections – Botox or Aimovig
- Lighting – limit exposure to fluorescent and blue lighting from screens
- Acupuncture
- Meditation
- Massage
- Physical Therapy
- Sleep Study
- CBD Oil
Lifestyle Recommendations to Lessen Migraines
- Sleep – get 8 continuous hours
- Diet – eat three healthy meals a day on a consistent schedule. Unhealthy foods can increase blood pressure and contribute to headaches.
- Personal Trigger Foods – avoid alcohol, caffeine, sugar, gluten, dairy or preserved meats, which can trigger symptoms. This is based on personal reactions to these foods.
- Hydration – drink 8 glasses of water a day. And remember that alcohol can cause dehydration.
- Exercise – releases neurotransmitters that reduce pain, aid circulation, and improve mood and sleep patterns.
Source: Amanda Harbert, CRNP, Carroll Health Group Neurology













